Blog
What Does Software As A Service Mean For Healthcare?
Nick Lucas is Senior Vice President of Professional Services and Site Leader for EMEA at Medidata Solutions.
Read more: What Does Softwar...Join Startups Magazine, virtually, to celebrate the launch of our first issue of the year, Finance & Fintech
Lets get Money Savvy: Different ways to Fund your Startup Date And Time: Tue, January 26, 2021 3:00 PM – 4:30 PM CET This will be a VIRTUAL event, held on Zoom but with a mix of polls and interactions.…
Read more: Join Startups Mag...The Covid-19 Pandemic And The Case For Healthcare As A Fundamental Freedom
Dr. Vanessa Kerry, cofounder and CEO of Seed Global Health, explains why the U.S. should take a rights-based approached to healthcare as a pillar of society on the anniversary of President Franklin Delano Roosevelt’s famous “Four Freedoms” speech.
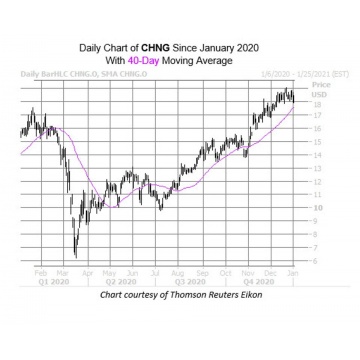
Read more: The Covid-19 Pand...Healthcare Stock Ready For Fresh Highs In 2021
Tech platform Change Healthcare (CHNG) enjoyed a sizable rally during the second half of 2020, steadily chugging past its pre-pandemic peak in mid-November to notch a Dec. 23 all-time-high of $19.08. Since then, the stock seems to have plateaued, with the $19 mark moving in as a ceiling in recent weeks. However, a pullback to a historically bullish trendline could keep some wind at the equity’s back, and even push it past this resistance level to register even more record highs in 2021.
Read more: Healthcare Stock ...Putting The Consumer At The Center Of Healthcare
It was not that long ago when it was heresy to talk about the consumer and healthcare in the same sentence. We, as consumers, did not help the situation. Many of us did not feel we knew that much about healthcare. It was generally something that was ‘done’ to us. As a result, we did not feel we had ‘standing’ or the ‘right’ to talk about it with the professionals to whom we entrusted our well-being. And a lot of the healthcare professionals whose advice we sought did not think we knew that much about it either. Some of them were quite happy keeping it that way. After all, the medical community had the language of science on its side. It was highly technical. It was obscure to most of us… and it was scary. So, many of us learned NOT to ask questions and basically do what we were told by the healthcare professionals we trusted.
Read more: Putting The Consu...Connecting the Dots: The Value of Partnerships in The Diabetes Industry | by April Huang, Senior Director New Business and Domain Portfolio, Ascensia Diabetes Care
As we prepare to attend the GIANT Health Event 2020 later this week, we have been looking at the leaders in healthcare innovation and the exciting start-ups that will be on show again this year. And the reason this type of event is interesting for us as a company in diabetes is simple. We do not believe that the challenges in diabetes can be overcome by one company working alone.
Read more: Connecting the Do...This year, we are celebrating and championing the world's best innovators, entrepreneurs, and businesses within healthcare technology
Over the years, there have been numerous outstanding achievements within healthcare that have improved the lives of millions worldwide and healthcare entrepreneurs, businesses, and visionaries, have been at the forefront of these achievements. Join us on Wednesday the 2nd of December,…
Read more: This year, we are...Tune in TODAY at 5pm for the next #BHHSeries
Barcelona Health Hub and AstraZeneca Foundation are hosting a #BHHSeries on telemedicine. The event will be opened by D. Alfredo González Gómez, Secretary General of Digital Health, Information and Innovation of the National Health System of MoH (Ministerio de España), which will explain the new Digital Health…
Read more: Tune in TODAY at ...GJE's Chartered Patent Attorney, Elizabeth Capel, takes a look at female led HealthTech patent trends
The global women’s health market is now expected to be worth $51.3 billion by 2025. Over the past 20 years, female participation in patent applications has increased to the extent that over one in five patents now have at least…
Read more: GJE's Chartered P...Invest in Skane will be attending our Giant Health event 1-2 December!
Invest in Skane are the official trade & investment promotion agency for the southernmost part of Sweden, Skåne. Stay tuned for more information!
Read more: Invest in Skane w...Only 5 days left of Early Bird prices
Buy your tickets to the GIANT HEALTH EVENT 2020 now before prices increase on November 8th. Don’t miss this incredible opportunity to see our fireside chat with VODAFONE at a discounted price! Buy ticket here.
Read more: Only 5 days left ...It's showtime! Join Barcelona Health Hub TODAY October 29th for the #BHHSummit!
Organized by Barcelona Health Hub Don't miss this chance to join this leading event in #digitalhealth. Forgot to book your ticket? No worries, you can still sign up for free here
Read more: It's showtime! Jo...